

Published on April 1, 2026 By 800ZED

You have had that feeling before. The stomach that churns before a stressful presentation. The appetite that disappears completely when you are heartbroken. The loose bowels before something terrifying.
We usually chalk these up to nerves. A physical reaction to an emotional state. But what if the relationship runs deeper than that? What if your gut is not just reacting to your emotions but actually helping to create them?
That is exactly what a rapidly growing body of research is now suggesting. And it is changing the way scientists, doctors, and nutritional psychiatrists think about mental health, anxiety, depression, and brain function in ways that would have seemed far-fetched just a decade ago.
The gut and the brain are in constant, two-way conversation. What happens in one affects the other ...and for millions of Filipinos whose daily diets and stress levels are quietly disrupting that conversation, the implications are significant.
This is not a metaphor. It is biology.
Your gut contains what scientists call the enteric nervous system, a vast network of over 500 million nerve cells lining your gastrointestinal tract from your esophagus to your rectum. It is so complex and so functionally independent that researchers began referring to it as the "second brain" decades ago. It can sense, process, and respond to information without any input from the brain in your head.
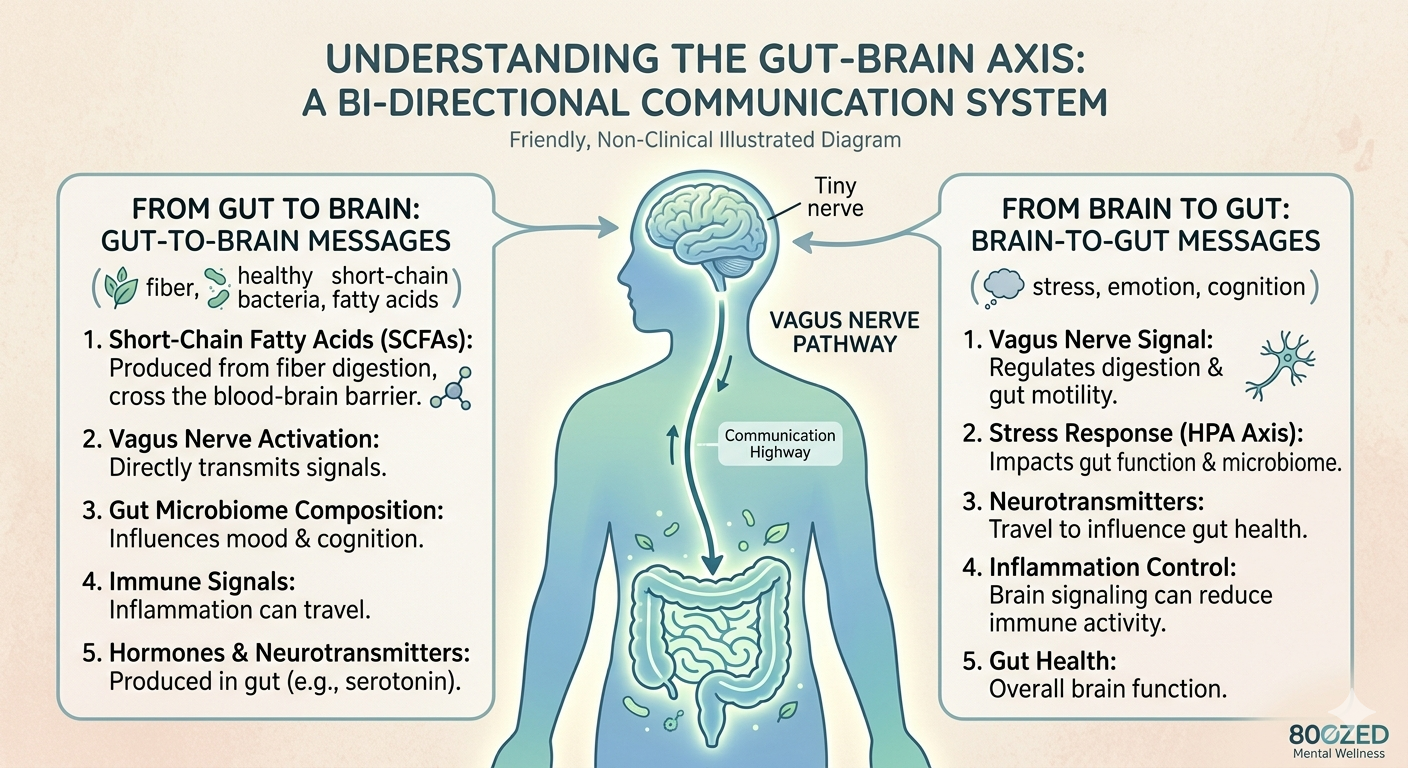
And then there is the gut-brain axis, the two-way communication highway that connects this second brain to your central nervous system. Information travels constantly in both directions through neural pathways including the vagus nerve, through hormones, through immune signaling, and through the chemical compounds produced by the trillions of microorganisms living in your digestive tract.
Those microorganisms — your gut microbiome — are not passive passengers. They are active participants in your neurological health. They produce neurotransmitter precursors. They regulate inflammation. They influence how your brain responds to stress. They help determine how much serotonin, dopamine, and GABA your body can produce and use.
Here is the number that tends to stop people in their tracks: approximately 90 to 95% of your body's serotonin is produced in your gut, not your brain. Serotonin is the neurotransmitter most closely associated with mood stability, feelings of wellbeing, and the regulation of anxiety. If your gut is unhealthy, inflamed, or populated with the wrong balance of bacteria, serotonin production can be significantly disrupted... and your mood will likely reflect that.
The research connecting gut health and mood has moved well beyond theoretical in recent years. The evidence is now substantial enough that a new field called nutritional psychiatry has emerged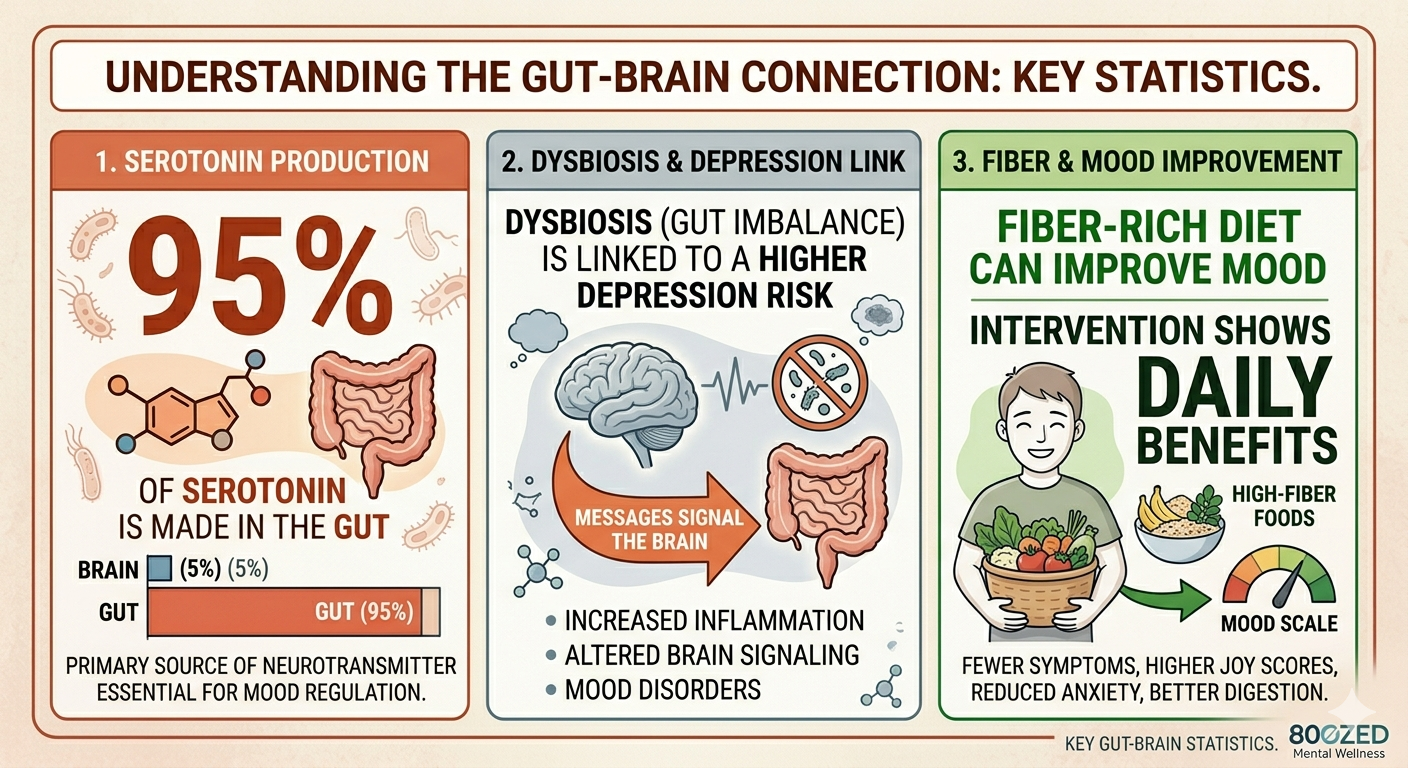 specifically to study and apply these connections clinically.
specifically to study and apply these connections clinically.
A 2025 review published in PMC found that
people with depression and anxiety
consistently show altered gut microbiome
composition compared to those without
these conditions. The disruption, known
as dysbiosis, reduces microbial diversity
and changes the balance of bacteria in ways that affect neurotransmitter production, immune function, and the brain's ability to adapt to stress. This connection is especially significant in the Philippines, where depression in young Filipinos has more than doubled in less than a decade — and the gut may be playing a bigger role in that crisis than most people realize.
A landmark study published in Nature in 2025 confirmed that the gut-brain axis has significant implications not just for mood disorders but for neurodegenerative and psychiatric conditions more broadly, including anxiety, depression, and even conditions like Parkinson's disease. The researchers noted that vagus nerve signaling from the gut is heavily implicated in regulating anxiety, learning, memory, and motivation.
Perhaps most striking for people looking for practical applications: a study published in 2025 found that a dietary fiber intervention, specifically increasing prebiotic fiber intake, measurably improved mood in everyday life among healthy adults. This was one of the first studies to demonstrate that what you eat can directly alter how you feel day to day, not through placebo, but through genuine changes in gut microbial activity.
A 2025 TIME report summarized the growing consensus among gastroenterologists and neuroscientists: "There is now more scientific proof than ever of a direct link between gut health and brain health. The gut microbiome can absolutely impact neuronal function."

Understanding that the gut affects the brain is one thing. Understanding what damages the gut in the first place is what makes the information actionable.
A low-fiber, highly processed diet.
Your gut bacteria feed primarily on dietary fiber from plants. When your diet is low in fiber and high in ultra-processed foods, refined carbohydrates, and sugar, the beneficial bacteria in your gut are literally starved. Their populations shrink. Less beneficial and more inflammatory bacterial strains take over. That shift in microbial balance, called dysbiosis, has direct downstream effects on mood, cognition, and stress resilience.
Stress does not just affect the brain. It directly alters the composition of the gut microbiome. Stress hormones like cortisol change the gut environment in ways that reduce microbial diversity
and increase intestinal permeability.
A leaky gut allows inflammatory molecules to enter the bloodstream, travel to the brain, and trigger neuroinflammation — which worsens symptoms of depression and anxiety in a reinforcing cycle.
For young Filipinos already dealing with burnout in their 20s, creates a compounding effect that quietly damages both mental and digestive health at the same time — often without either being recognized for what it is.
Antibiotics and medications.
Antibiotics are lifesaving and sometimes essential, but they do not discriminate between harmful bacteria and the beneficial microbes your gut depends on. A single course of antibiotics can significantly reduce gut microbial diversity, with effects that can persist for months without deliberate dietary support to rebuild the microbiome.
Poor sleep.
The gut microbiome follows circadian rhythms just like the rest of the body. Disrupted sleep patterns alter microbial activity and reduce the production of beneficial short-chain fatty acids that support gut lining integrity and brain function. This is one reason why sleep deprivation so reliably worsens mood and cognitive function beyond just tiredness.
Alcohol.
Excessive alcohol consumption disrupts the balance of gut bacteria, increases intestinal permeability, and drives inflammation in ways that directly affect mood. The temporary mood lift that alcohol provides is followed by neurological and gut disruption that compounds anxiety and low mood in the days after drinking.
The Filipino diet and lifestyle create some specific gut health challenges worth naming honestly.
 The rice and refined carbohydrate staple.
The rice and refined carbohydrate staple.
White rice is a cultural cornerstone
of Filipino eating. On its own, it is
not inherently harmful. But a diet
where white rice dominates nearly
every meal, often alongside processed
meats, fried foods, and sweet drinks,
with relatively limited vegetable and
fiber variety, creates a gut environment that struggles to maintain microbial diversity.
This dietary pattern does not just affect the gut. It is also one of the primary drivers of insulin resistance in Filipino women — another silent condition that disrupts hormones, mood, and energy in ways that compound the effects of poor gut health over time.
Rising stress and mental health burden.
Workplace surveys show Filipino employees rank among the most stressed in Southeast Asia. The AXA 2025 Mind Health Report found that financial pressure, job insecurity, and loneliness are chronic stressors for young Filipinos. Chronic stress, as the research shows, directly damages the gut microbiome. The mental health crisis and the gut health challenge in the Philippines are not separate problems. They feed each other.
Limited probiotic and fermented food culture.
Many Asian food cultures have strong fermented food traditions, kimchi in Korea, miso and natto in Japan, tempeh in Indonesia. Fermented foods are natural sources of beneficial bacteria that support gut microbiome diversity. Filipino cuisine has far fewer of these staples integrated into daily eating, meaning many Filipinos miss out on a consistent natural source of probiotic support.
Awareness is growing, but slowly.
In 2026, gut health has become the number one wellness theme driving nutrition choices among Filipino consumers, according to SunStar Davao's wellness report. More Filipinos are adding fiber-rich foods and supplements to their diets and starting to connect digestive health to overall wellbeing. But the connection between gut health and mental health specifically is still not widely understood or discussed in everyday Filipino health conversations.
This is not always obvious, because the gut-mood connection works slowly and cumulatively rather than dramatically. But watch for these patterns:
You feel anxious or low without a clear reason. Not linked to a specific stressor or event, just a baseline unease or flatness that does not fully go away.
Your mood crashes after eating. Particularly after carbohydrate-heavy or processed meals. This can reflect both blood sugar fluctuations and gut bacterial responses to food.
You have persistent digestive issues alongside mood problems. Bloating, irregular bowel movements, IBS-type symptoms, and frequent stomach discomfort often co-occur with anxiety and depression because both share the same underlying gut disruption.
You feel mentally foggy and unfocused. Brain fog is one of the most reported symptoms of poor gut health, linked to neuroinflammation caused by dysbiosis and leaky gut.
Your mood seems to worsen after a course of antibiotics. This is not imagination. Antibiotics significantly disrupt gut microbial diversity, and that disruption can affect mood for weeks to months afterward if the microbiome is not actively supported.
You crave sugar and refined carbs constantly. Certain bacterial strains that thrive on sugar actively signal the brain for more of what they feed on. Strong, persistent carbohydrate cravings can be a sign that less beneficial bacteria are dominating your gut environment.
The good news here is genuinely encouraging. The gut microbiome is not fixed. It responds to changes in diet and lifestyle relatively quickly, and improvements in gut health have been shown to produce measurable changes in mood and cognitive function within weeks.

Eat more fiber, and vary your plants.
This is the single most impactful change you can make for gut microbiome health. Gut bacteria feed on dietary fiber, and different bacterial strains thrive on different types of plant fiber. The goal is not just more fiber but more variety. Aim for a wider range of vegetables, fruits, legumes, and whole grains across the week. Oats, beans, bananas, garlic, onions, and leafy vegetables are all excellent sources of prebiotic fiber that specifically feed beneficial gut bacteria.
Add fermented foods.
Yogurt with live cultures, fermented vegetables, kefir, kimchi, and other naturally fermented foods introduce beneficial bacterial strains directly into the gut. You do not need to eat large amounts. Even small, consistent daily servings of fermented food can measurably support microbial diversity over time.
Reduce ultra-processed food and refined sugar.
Not as a punishment, but because these foods actively feed the less beneficial bacterial strains and starve the ones that support mood and brain health. A gradual, sustainable reduction has more long-term impact than a dramatic short-term elimination.
Manage stress actively.
Because stress damages the gut directly, stress management is not just a mental health strategy. It is a gut health strategy. Walking, breathing exercises, adequate sleep, meaningful social connection, and reducing chronic overcommitment all protect the gut microbiome in ways that eventually feed back into better mood regulation.
Prioritize sleep consistency.
Going to bed and waking at consistent times supports the circadian rhythms that the gut microbiome depends on. Even when you cannot get more sleep, getting more consistent sleep is a meaningful step.
Consider probiotics, but choose thoughtfully.
Probiotic supplements vary enormously in quality, strain specificity, and clinical evidence. Not all probiotics are equally effective for mood-related benefits. If you are considering supplementation, speaking to a doctor first helps ensure you are choosing something with actual evidence behind it for your specific situation rather than just the most heavily marketed option.
Limit alcohol.
Even moderate, regular alcohol consumption disrupts the gut microbiome in ways that compound anxiety and low mood over time. Reducing intake, even partially, has measurable gut health benefits relatively quickly.
Here is what makes the gut-brain connection so important to understand right now, especially in the Philippines where both mental health challenges and diet-related health issues are growing simultaneously.
Mental health is not only about what happens in the brain. It is about the whole system — the food you eat, the stress you carry, the sleep you get, the bacteria that live in your digestive tract and communicate with your nervous system every single day.
This does not mean that depression or anxiety can be cured by eating more vegetables. Clinical mental health conditions require clinical support, and anyone struggling with persistent low mood, anxiety, or burnout should speak to a doctor. But it does mean that the food choices you make every day are not neutral when it comes to how you feel. They are part of the picture in ways that science is only beginning to fully map.
Taking care of your gut is not a wellness trend. It is one of the most direct ways you can take care of your brain.
If you have been struggling with mood, energy, or mental clarity and want to understand what might be contributing, a telemedicine consultation or clinic visit with 800Zed can help you assess your overall health picture, including gut and metabolic health, and build a plan that actually works for your lifestyle.
Book a consultation today: https://800zed.com
Frontiers in Microbiomes. The gut-brain connection: microbes' influence on mental health. 2025. https://www.frontiersin.org/journals/microbiomes/articles/10.3389/frmbi.2025.1701608/full
TIME Magazine. Your Gut Could Be Affecting Your Mood. November 2025. https://time.com/7329016/gut-health-foods-brain-mood/
Nature. Gut-brain axis and neuropsychiatric health: recent advances. January 2025. https://www.nature.com/articles/s41598-025-86858-3
PMC. The Gut-Brain Axis and Mental Health: How Diet Shapes Our Mood
_______________
Stay connected with the 800ZED Blog! Get the latest health tips, wellness insights, and simple daily habits that can boost your well-being — from your sleep routine to your screen time. Subscribe now and take small steps toward a healthier, happier you.
We use cookies to give you the best service on our site. By continuing to use the site you consent to our Privacy Policy
📲 Install 800 ZED App for quick access!
📲 Install 800 ZED App on your iPhone
Tap Share → Add to Home Screen
📲 Install 800 ZED on Firefox
Open menu ☰ → Install
Subscribe our newsletter for latest updates
Get the latest updates, promotions, and news delivered straight to your inbox.